  
This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". The cookie is used to store the user consent for the cookies in the category "Analytics". 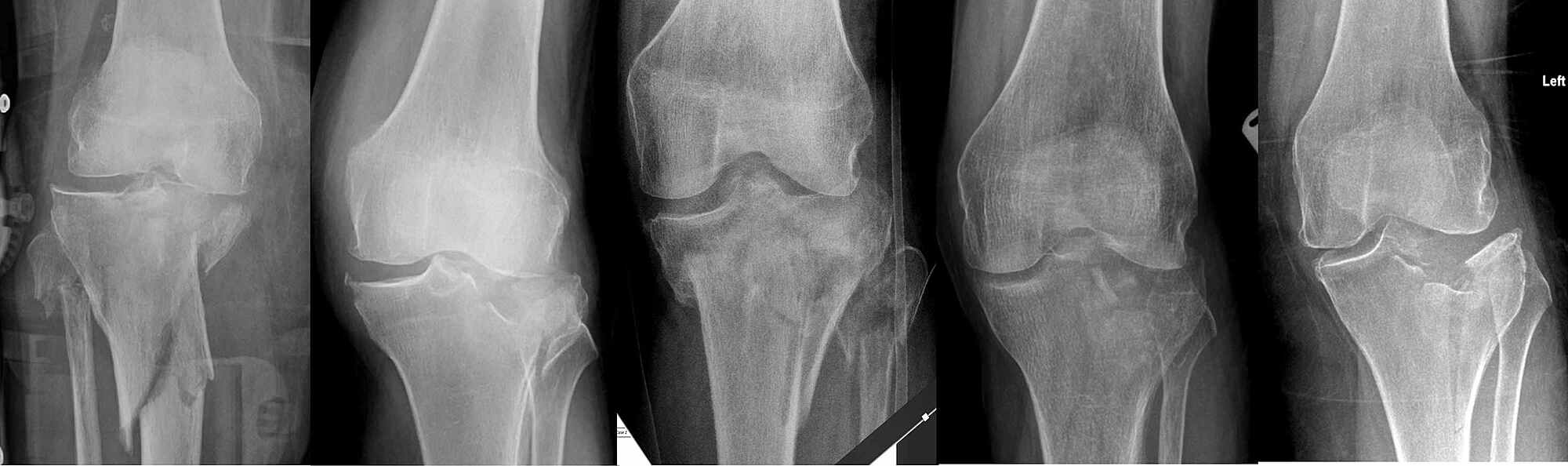
These cookies ensure basic functionalities and security features of the website, anonymously. Necessary cookies are absolutely essential for the website to function properly. The main long-term complication following a tibial plateau fracture is post-traumatic osteoarthritis to the affected joint. * Complicated fractures include those demonstrating an articular step ≥2mm, angular deformity ≥10 degrees, any metaphyseal-diaphyseal translation, ligamentous injury requiring repair, or those with associated tibial fractures Complications Figure 3 - CT imaging demonstrating lipohaemarthrosis due to a tibial plateau fracture Operative Management * It is important to recognise that the presence of fat in the joint indicates that there is an intra-articular fracture present (e.g. This help both in assessment of severity, as well as surgical planning. There will also be a lipohaemarthrosis present.ĬT scanning is needed in almost all cases (Fig. The first line investigation for a suspected plateau fracture is plain film radiographs (anteroposterior and lateral), often features on radiograph are subtle (Fig. * This represents a lipohaemarthrosis and is an important clinical and radiological feature to recognise Differential Diagnosisįor patients presenting with knee pain following trauma, other differentials to consider are knee dislocation, other knee fractures (including patella or distal femur), meniscal injuries, ligamentous injuries, patella dislocation, or patella/quadriceps tendon rupture. On examination, significant swelling will be evident, alongside tenderness over the medial or lateral aspects of the proximal tibia, with potential ligament instability (albeit not clinically assessed initially, due to the pain it would cause).Įnsure to check peripheral neurovascular status of the patient, as neurovascular injuries (such as popliteal vessel dissection or common fibular nerve damage) are an important association of high grade injuries. Patients will present with sudden onset pain in the affected knee, being unable to weight-bear, and swelling of the knee*. A clear history of the mechanism of injury is important, as an injury through axial loading or high-impact injuries will increase the likelihood of a tibial plateau fracture. Patients will present following a history of trauma. Figure 1 - The tibial plateau Clinical Features * Complicated fractures include those demonstrating an articular step ≥2mm, angular deformity ≥10 degrees, any metaphyseal-diaphyseal translation, ligamentous injury requiring repair, or those with associated tibial fractures Postoperatively, a hinged knee brace is fitted with early passive range of movement but limited or non-weight bearing for around 8-12 weeks months is typically required.Įxternal fixation with delayed definitive surgery is indicated in cases of significant soft tissue injury, polytrauma and highly comminuted fractures where an immediate ORIF may not be suitable. Any metaphyseal gaps can be filled with bone graft or bone substitute. Open reduction and internal fixation (ORIF) is the mainstay of most tibial plateau fractures, with the aim to restore the joint surface congruence and ensure joint stability. Any form of medial tibial plateau fractures may also require surgical intervention, even if undisplaced, as they have a great potential for displacement. Operative management is typically warranted in complicated tibial plateau fractures*, or any evidence of open fracture or compartment syndrome. 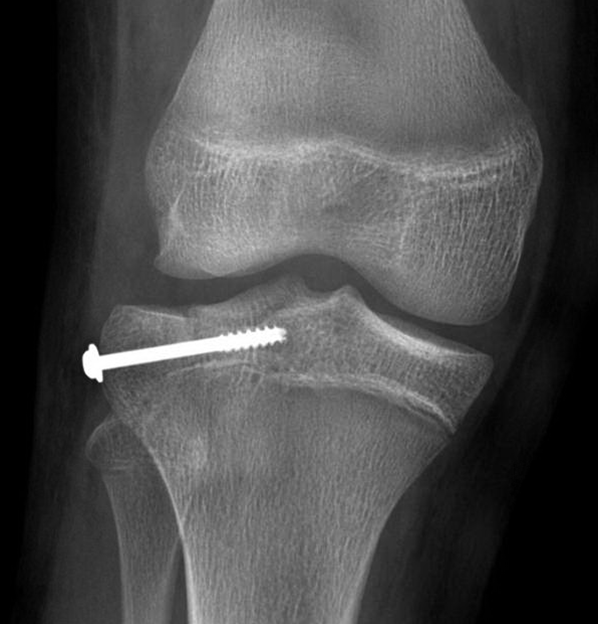
Figure 3 – CT imaging demonstrating lipohaemarthrosis due to a tibial plateau fracture Operative Management 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
